BIPOLAR DISORDER
Bipolar disorder (once called manic depression or bipolar depression) is a mental health condition which is characterised by extreme mood changes – someone with this disorder may be very ‘high’ and over-excited or very ‘low’ and depressed, often with periods of normal moods in between. The extreme nature of the condition means staying in a job may be difficult and relationships may become strained. Men and women are equally likely to develop bipolar disorder.
People with bipolar disorders are at very high risk of death by suicide. The incidence of death by suicide among people with bipolar disorder is high, particularly when bipolar disorder is untreated
However, there are effective treatments to help manage the symptoms of bipolar disorder. Proper diagnosis and treatment help people with bipolar disorder lead healthy and productive lives.
There are two types of bipolar disorders:
- Bipolar 1 disorder
- Bipolar 2 disorder
Bipolar 1 disorder
Bipolar 1 disorder is diagnosed when a person has experienced a manic episode. Neither psychosis or a current or past major depressive episode is required for a Bipolar 1 disorder diagnosis.
Development
The average age of onset for bipolar 1 disorder is approximately 18 years. Approximately 60% of manic episodes occur immediately before a major depressive episode.
Prevalence
“It is estimated that the lifetime prevalence rate of bipolar 1 disorder 0.6%.
Bipolar 2 disorder
Bipolar 2 disorder is diagnosed when a person has experienced a current or past hypomanic episode and a current or past depressive episode. Although Hypomania is a less severe form of mania, Bipolar 2 disorder is equally as debilitating as Bipolar 1 disorder. People with Bipolar 2 disorder tend to experience depressive episodes more often and the instability in mood ("highs" and "lows") interferes significantly with social and occupational functioning.
Prevalence
“It is estimated that the lifetime prevalence rate of bipolar 2 disorder is 0.4%.
Manic Episode
Having a manic episode can sometimes feel exciting and fun, but it can also feel distressing, disorientating or unpleasant. Manic episodes are not just how an "energetic" or "hyper" person behaves but is drastically different from the moods and behaviours that are typical for the person. This episode also is severe to interfere with the person's social and occupational functioning or requires hospitalisation to prevent harm to the self or to others.
Common symptoms of mania include:
- Feel very “up,” “high,” or elatedness
- Have a lot of energy
- Have increased activity levels
- Feel “jumpy” or “wired”
- Not feeling like sleeping
- Become more active than usual
- Talk really fast about a lot of different things
- Be agitated, irritable, or “touchy”
- Easily distracted
- Feel like their thoughts are going very fast
- Think they can do a lot of things at once
- Do risky things, like spend a lot of money or have reckless sex
- Making decisions or saying things that are out of character and that others see as being risky or harmful
This mood is present nearly every day for at least a week but episodes of mania can sometimes last for several weeks.
Hypomanic Episode
Although common symptoms of hypomania and mania are the same, there are some key differences.
Hypomanic symptoms are likely to:
- feel more manageable – for example, you might feel able to go to work and socialise without any major problems (although people might still notice your change in mood).
- last for a shorter time (at least nearly every day, most of the day for 4 days)
- not include any psychotic symptoms
Hypomanic episodes, like manic episodes, is noticeably different from how the person usually behaves. While the duration of a hypomanic episode is shorter than a manic episode, a hypomanic episode can still have a significant impact on someone's life and be very difficult to cope with.
Major Depressive Episode
Many people find that a depressive episode can feel harder to deal with than manic or hypomanic episodes. The contrast between your high and low moods may make your depression seem even deeper.
Common symptoms of depression include:
- feeling sad, hopeless or irritable most of the time
- lacking energy
- difficulty concentrating and remembering things
- loss of interest in everyday activities
- feelings of emptiness or worthlessness
- feelings of guilt and despair
- feeling pessimistic about everything
- self-doubt
- being delusional, having hallucinations and disturbed or illogical thinking
- lack of appetite
- difficulty sleeping
- waking up early
- suicidal thoughts
A depressive episode lasts most days, nearly every day, for at least 2 weeks. This feeling down makes it tremendously difficult for a person to function in social, occupational and other important life domains.
Prevalence
The prevalence rate of bipolar disorders in Malaysia is unknown. Further research is needed to establish how prevalence bipolar disorders are in Malaysia. The prevalence rate reported here are taken from studies conducted mostly in Western cultures, and where available, Asian cultures like Singapore.
Development
The average age of onset of bipolar 2 disorder is mid-20s. Many people with bipolar 2 disorder experience a depressive episode first before a hypomanic episode occurs.
Sometimes people with severe episodes of mania or depression experience psychotic symptoms such as hallucinations or delusions. The psychotic symptoms tend to match the person’s extreme mood. For example:
- Someone having psychotic symptoms during a manic episode may believe she is famous, has a lot of money, or has special powers.
- Someone having psychotic symptoms during a depressive episode may believe he is ruined and penniless, or that he has committed a crime.
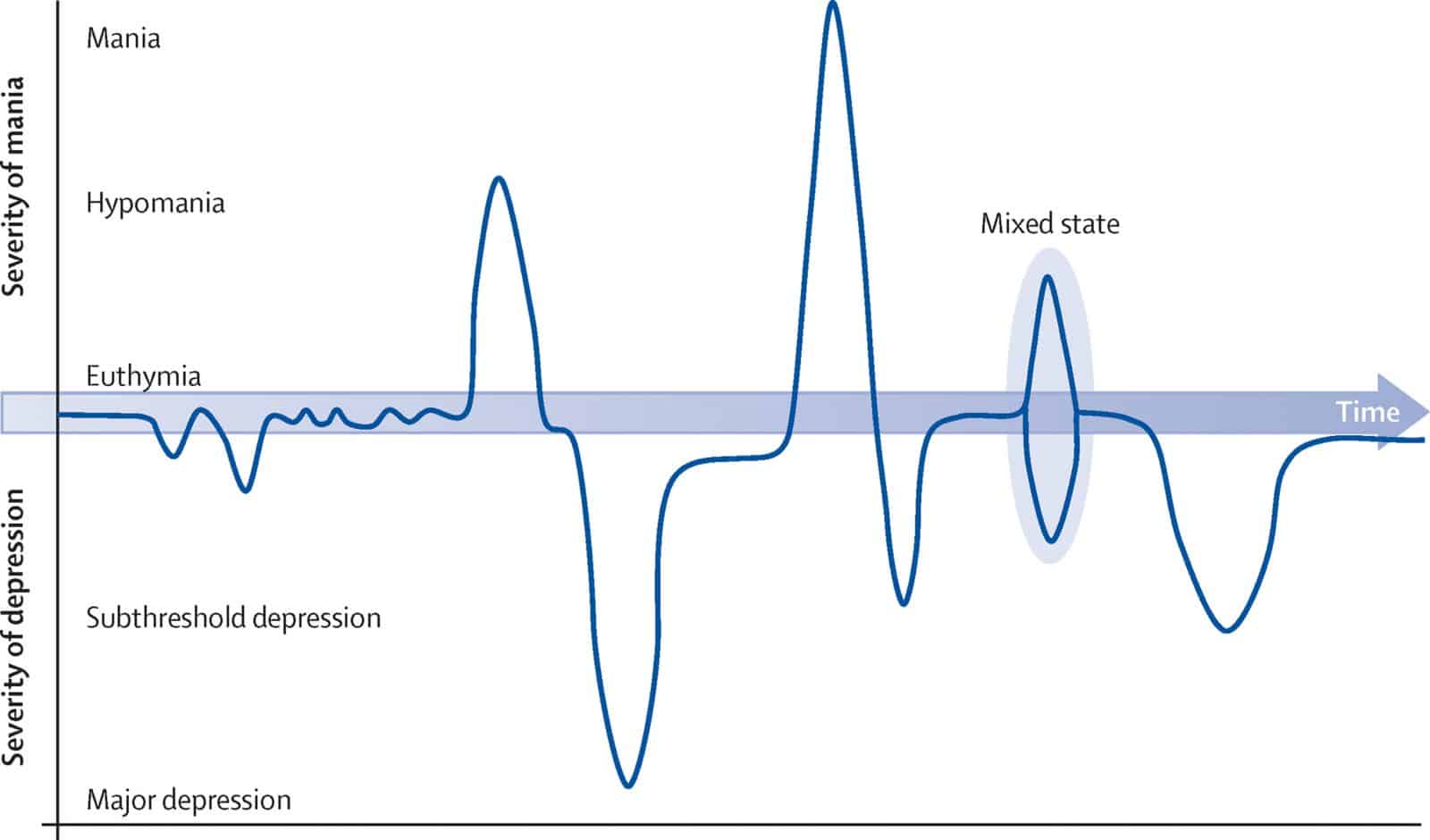
*Euthymia refers to normal mood state.
Life chart showing the progression of bipolar disorder taken from Grande, Berk, Birmaher & Vieta, 2016.
References
- Grande, I., Berk, M., Birmaher, B., & Vieta, E. (2016). Bipolar disorder. The Lancet, 387(10027), 1561-1572.
- Merikangas, Kathleen R. et al. “Prevalence and Correlates of Bipolar Spectrum Disorder in the World Mental Health Survey Initiative.” Archives of general psychiatry 68.3 (2011): 241–251. PMC. Web. 14 Apr. 2017.
- https://www.nimh.nih.gov/health/topics/bipolar-disorder/index.shtml
- http://www.mind.org.uk/information-support/types-of-mental-health-problems/bipolar-disorder/#.WPCDdlN95sM
- http://www.nami.org/Learn-More/Mental-Health-Conditions/Bipolar-Disorder
- http://www.cmha.ca/mental-health/understanding-mental-illness/bipolar-disorder/
- https://www.sane.org/mental-health-and-illness/facts-and-guides/bipolar-disorder

