In the past week, there has been a great deal of attention on the incarceration of certain prominent activists, leading many Malaysians to protest against SOSMA and its application. Since 2000, the prison population in Malaysia has doubled and many of these offenders do not have anyone to speak up on their behalf.
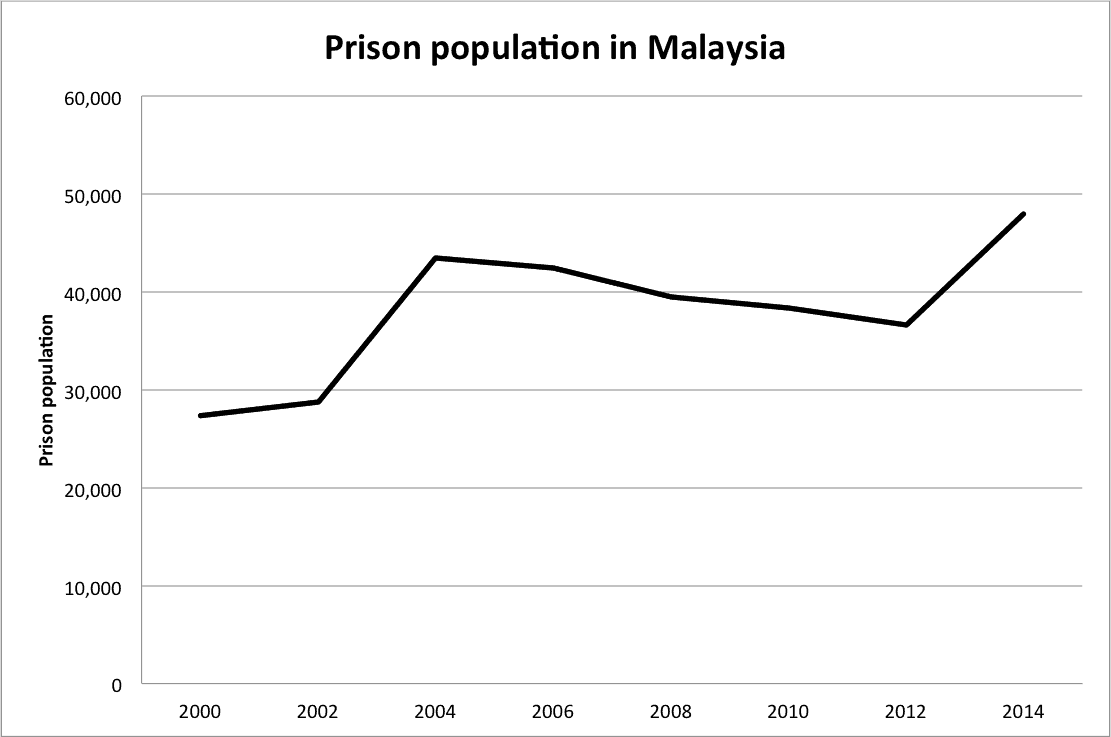 Taken from http://www.prisonstudies.org/country/malaysia
Taken from http://www.prisonstudies.org/country/malaysia
You may have heard in the news that the mentally ill are over-represented in prison. The Bureau of Justice Statistics of USA estimated that 56% of State prisoners, 45% of Federal prisoners, and 64% of jail inmates have a mental illness in the USA. But this is not just an American problem – UK, Australia and Canada also report similar statistics. In two meta-analysis which analyzed all available data in over 20 countries worldwide on the prevalence of mental illness in prisoners, found an an overall prevalence rate of 3.7% for psychotic illness, 11.4% for major depression and 65% for amongst prisoners (Fazel & Fanesh, 2002; Fazel & Seewalk, 2012)1. This is 2 – 4 times the prevalence rate in the general population (1% for schizophrenia and 5% for depressive disorders).
This is a worldwide problem.
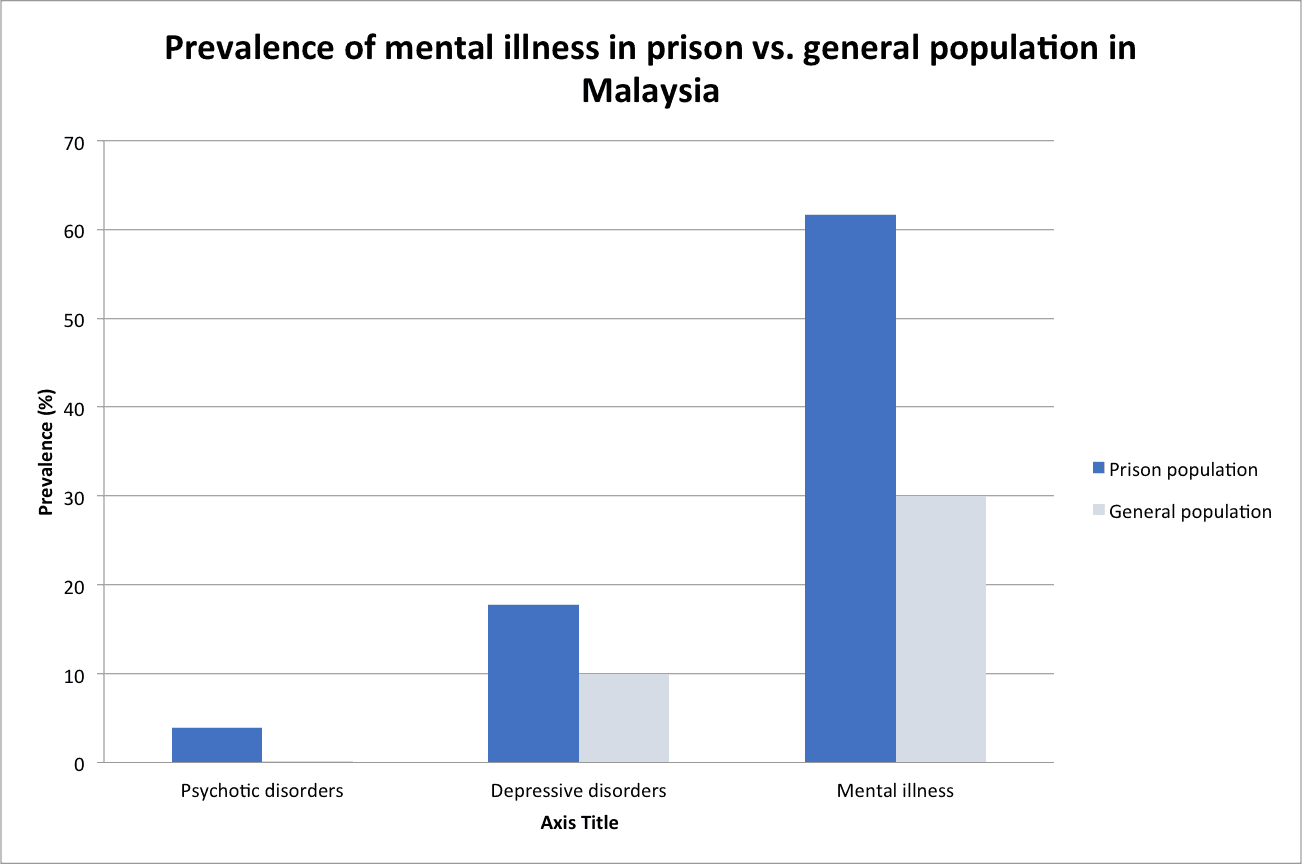
1. There is a higher prevalence for mental illness among the prison population than the general population in Malaysia.
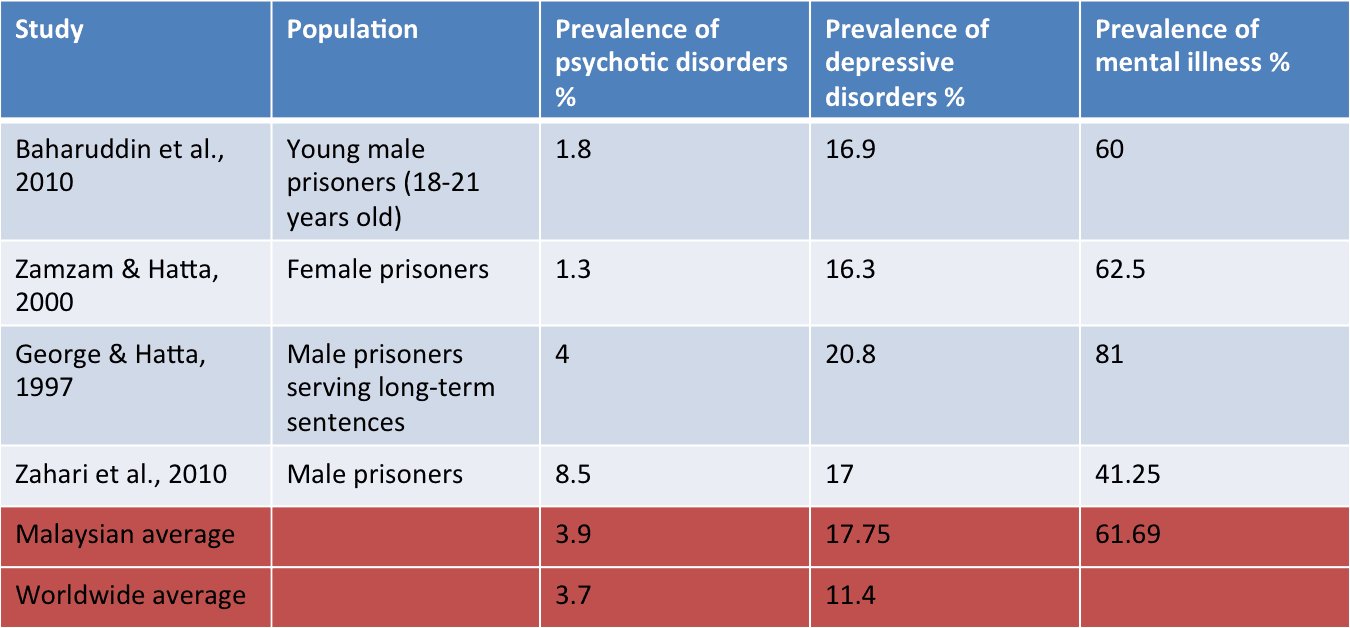
There is no official data on the mental health data of prisoners in Malaysia. However, even though the Malaysian Prison Department has not released the official statistics on the health of prisoners, several studies have been conducted looking at psychiatric disorders among prisoners in Malaysia.
Ignoring the differences between studies and focusing on the average prevalence rate across studies, we find that the prevalence rate for psychotic disorders is relatively comparable to what was found world-wide, but significantly higher for depressive disorders.
Given that:
i.The estimated prevalence of depressive disorders in Malaysia is 10% (Ng, 2014)
ii.The estimated prevalence of schizophrenia in Malaysia is .24% (Simeone, Ward, Rotella, Collins, & Windisch, 2015).
iii.The prevalence of mental illness in Malaysia is 30% (National Comorbidity and Health Survey, 2015).
the approximated prevalence of mental illness for Malaysian prisoners based on available data is reasonable. It is also consistent with the global finding that the prevalence of mental illness for prisoners is 2 – 4 times higher than the prevalence rate in the general population.
2. Mental disorders are not necessarily the cause of violence. Individuals who are mentally ill are far more likely to be a victim of violence than to be violent.
There is a common fear that mental illness is associated with violence. Given the higher prevalence of mental illness in the prison population as compared to the general population, one might be tempted to conclude that the rate of incarceration of the mentally ill accurately reflects their propensity towards violence.
This is a complicated issue and research often presents mixed findings. Some studies show no relationship between mental illness and crime while others do. Overall, it appears that mental illness is a small risk factor for violence (Mulvey, 1994; Glied & Frank, 2014). It increases the risk, but mental illness is not a determining factor for violence.
The stigma against mental illness and the strong association between mental illness and crime is disproportionate to the actual risk. Not all individuals who commit a crime have a mental illness and not all individuals who are mentally ill commit crimes. Mental illness is but one factor among many others to consider in risk assessment.
Moreover, even though psychotic disorders are associated with violence, the symptoms themselves are not directly related to crime (Peterson et al., 2014). In a study that examined 429 crimes, only 4% were related to symptoms of schizophrenia, 3% to symptoms of depressive disorders and 10% to symptoms of bipolar disorders. Anger and social deviance are better predictors of criminal behaviour than of psychotic or depressive symptoms (Skeem, Kennealy, Monahan, Peterson & Appelbaum, 2016).
In fact, individuals who are mentally ill are 2 times more likely to be a victim of violence rather than being a perpetrator of violence (Maniglio, 2009) and 3 -6 times more likely to be a victim of physical and sexual violence compared to someone without a mental illness (Khalifeh, Oram, Osborn, Howard, & Johnson, 2016).
3. Possible reasons for the high number of individuals who are mentally ill in the criminal justice system.
- Individuals who are mentally ill are stigmatized against and charged in the criminal justice system even for minor offenses because they are deemed dangerous due to their mental illness.
- Police are not sufficiently trained to dealing with mental illness and may wrongly perceive the state of psychosis as alcohol or drug intoxication.
- Police are not sufficiently trained or Malaysian hospitals are not sufficiently equipped to deal with individuals who may be experiencing a psychosis or mania, or in a particularly vulnerable state. Therefore they resort to using prison as a holding place.
- Restrictive laws such as Section 39 of the Penal Code which makes it illegal for someone to commit suicide means that individuals who are in psychological distress will end up in prison because they were in a state of hopelessness and attempted suicide.
- There is a lack of mental health care and understanding of mental illness in Malaysia. Only 20% of offenders who were mentally ill had received psychiatric care prior to their incarceration (Zahari et al., 2010). The lack of mental health care increases the risk of substance abuse, homelessness, poorer physical physical and mental health. In this state, they are unable to care for themselves and may find it difficult to control their impulses (e.g. a response to a persecutory delusion) and consequently commit a violent/criminal act.
- Mental illness is a risk factor for developing a substance abuse disorder or substance dependence (Buckner, Heimberg, Schneier, Liu, Wang, & Blanco, 2012; Davis, Compton, Wang, Levin & Blanco, 2013; Stone, Becker, Huber, & Catalano, 2012). The criminalization of drug use under the Dangerous Drugs Act 1952 increases the chances that individuals suffering from a mental illness will be incarcerated due to substance use, rather than violence. Indeed, about 60% of prisoners in Malaysia are charged with a drug-related offense (Mazlan et al., 2006).
Due to the stigmatization of mental illness and attention-grabbing headlines, much of the attention has been on the association between mental illness and violence. The dark side of mental illness is not that individuals who are mentally ill will be violent, but rather they will be violated and victimized far more frequently than someone without a mental illness. We need to look for better solutions for individuals who are mentally ill – solutions that will actually help them and not hurt them, solutions that will provide them the mental health care that they need and deserve as a fundamental human right.
References
Baharuddin, A., Yusof, M., Akhtar, S., Nik Jaafar, N. R., & Zakaria, H. (2010). Psychiatric disorders among young male adult prisoners: a cross sectional study in a Malaysian prison. Malaysian Journal of Medicine and Health Sciences, 6(2), 65-70.
Baillargeon, J., Binswanger, I. A., Penn, J. V., Williams, B. A., & Murray, O. J. (2009). Psychiatric disorders and repeat incarcerations: the revolving prison door. American Journal of Psychiatry, 166(1), 103-109.
Bonta, J., Blais, J., & Wilson, H. A. (2014). A theoretically informed meta-analysis of the risk for general and violent recidivism for mentally disordered offenders. Aggression and violent behavior, 19(3), 278-287.
Buckner, J. D., Heimberg, R. G., Schneier, F. R., Liu, S. M., Wang, S., & Blanco, C. (2012). The relationship between cannabis use disorders and social anxiety disorder in the National Epidemiological Study of Alcohol and Related Conditions (NESARC). Drug and alcohol dependence, 124(1), 128-134.
Davis, G. P., Compton, M. T., Wang, S., Levin, F. R., & Blanco, C. (2013). Association between cannabis use, psychosis, and schizotypal personality disorder: findings from the National Epidemiologic Survey on Alcohol and Related Conditions. Schizophrenia research, 151(1), 197-202.
DeLisi, M., Vaughn, M. G., Gentile, D. A., Anderson, C. A., & Shook, J. J. (2013). Violent video games, delinquency, and youth violence new evidence. Youth Violence and Juvenile Justice, 11(2), 132-142.
Douglas, K. S., Guy, L. S., & Hart, S. D. (2009). Psychosis as a risk factor for violence to others: a meta-analysis. Psychological bulletin, 135(5), 679.
Fazel, S., & Danesh, J. (2002). Serious mental disorder in 23 000 prisoners: a systematic review of 62 surveys. The lancet, 359(9306), 545-550.
Fazel, S., & Seewald, K. (2012). Severe mental illness in 33 588 prisoners worldwide: systematic review and meta-regression analysis. The British Journal of Psychiatry, 200(5), 364-373.
George, P., & Hatta, S. M. (1997). Prevalence Of Severe Mental Disorders Among Males Serving Long Term Sentences In A Malaysian Prison. Asean Journal Of Psychiatry, 5(2), 12-17.
Honegger, L. N. (2015). Does the evidence support the case for mental health courts? A review of the literature. Law and human behavior, 39(5), 478.
Khalifeh, H., Oram, S., Osborn, D., Howard, L. M., & Johnson, S. (2016). Recent physical and sexual violence against adults with severe mental illness: a systematic review and meta-analysis. International review of psychiatry, 28(5), 433-451.
Lamb, H. R., Weinberger, L. E., & Gross, B. H. (2004). Mentally ill persons in the criminal justice system: Some perspectives. Psychiatric Quarterly, 75(2), 107-126.
Maniglio, R. (2009). Severe mental illness and criminal victimization: a systematic review. Acta Psychiatrica Scandinavica, 119(3), 180-191
Mazlan, M., Mazlan, M., Schottenfeld, R. S., Mazlan, M., Schottenfeld, R. S., Chawarski, M. C., … & Chawarski, M. C. (2006). New challenges and opportunities in managing substance abuse in Malaysia. Drug and Alcohol Review, 25(5), 473-478.
Ng, C. G. (2014). A review of depression research in malaysia. The Medical journal of Malaysia, 69, 42-45.
O’Leary, K. D., Tintle, N., & Bromet, E. (2014). Risk factors for physical violence against partners in the US. Psychology of violence, 4(1), 65.
Peterson, J. K., Skeem, J., Kennealy, P., Bray, B., & Zvonkovic, A. (2014). How often and how consistently do symptoms directly precede criminal behavior among offenders with mental illness?. Law and Human Behavior, 38(5), 439.
Simeone, J. C., Ward, A. J., Rotella, P., Collins, J., & Windisch, R. (2015). An evaluation of variation in published estimates of schizophrenia prevalence from 1990─ 2013: a systematic literature review. BMC psychiatry, 15(1), 1.
Skeem, J., Kennealy, P., Monahan, J., Peterson, J., & Appelbaum, P. (2016). Psychosis uncommonly and inconsistently precedes violence among high-risk individuals. Clinical psychological science, 4(1), 40-49.
Steadman, H. J., Redlich, A., Callahan, L., Robbins, P. C., & Vesselinov, R. (2011). Effect of mental health courts on arrests and jail days: A multisite study. Archives of general psychiatry, 68(2), 167-172.
Stone, A. L., Becker, L. G., Huber, A. M., & Catalano, R. F. (2012). Review of risk and protective factors of substance use and problem use in emerging adulthood. Addictive behaviors, 37(7), 747-775.
Van Dorn, R., Volavka, J., & Johnson, N. (2012). Mental disorder and violence: is there a relationship beyond substance use?. Social psychiatry and psychiatric epidemiology, 47(3), 487-503.
Zahari, M. M., Hwan Bae, W., Zainal, N. Z., Habil, H., Kamarulzaman, A., & Altice, F. L. (2010). Psychiatric and substance abuse comorbidity among HIV seropositive and HIV seronegative prisoners in Malaysia. The American journal of drug and alcohol abuse, 36(1), 31-38.
Zamzam, R., & Hatta, S. M. (2000). Specific Psychiatric Disorders Among Convicted Female Offenders in a Malaysian Prison. Malaysian Journal of Psychiatry, 8(1), 34-42.
Footnotes
1
1. Psychotic disorders included schizophrenia spectrum and mania.
a. Schizophrenia:
Schizophrenia spectrum and other psychotic disorders include schizophrenia, other psychotic disorders, and schizotypal (personality) disorder. They are defined by abnormalities in one or more of the following five domains: delusions, hallucinations, disorganized thinking (speech), grossly disorganized or abnormal motor behavior (including catatonia), and negative symptoms.
Prevalence in general population 1%
Prevalence in prison population 3.7%
b. Mania:
A distinct period of abnormally and persistently elevated, expansive, or irritable mood, lasting at least 1 week (or any duration if hospitalization is necessary).
During the period of mood disturbance, three (or more) of the following symptoms have persisted (four if the mood is only irritable) and have been present to a significant degree.
- 1. inflated self-esteem or grandiosity
- 2. decreased need for sleep (e.g., feels rested after only 3 hours of sleep)
- 3. more talkative than usual or pressure to keep talking
- 4. flight of ideas or subjective experience that thoughts are racing
- 5. distractibility (i.e., attention too easily drawn to unimportant or irrelevant external stimuli)
- 6. increase in goal-directed activity (either socially, at work or school, or sexually) or psychomotor agitation
- 7. excessive involvement in pleasurable activities that have a high potential for painful consequences (e.g., engaging in unrestrained buying sprees, sexual indiscretions, or foolish business investments)
2. Depressive disorders:
Depressive disorders include disruptive mood dysregulation disorder, major depressive disorder and persistent depressive disorder (dysthymia). Depressive disorders are defined by the presence of sad, empty, or irritable mood, accompanied by somatic and cognitive changes that significantly affect the individual’s capacity to function.
Prevalence in general population 5%
Prevalence in prison population 11.4%
Dr. Chua Sook Ning is a Clinical Psychologist and a lecturer at the National Institute of Education at Nanyang Technological University, Singapore. She believes in raising public awareness of mental health by encouraging open and public conversations of mental health. She also is also working on early identification of mental health conditions by promoting mental health screenings and. training communities to recognize mental health conditions. Finally, she is working with a team of international researchers to develop accessible and affordable mental health interventions.




Pingback: Behind the Bars: A Look Inside the Malaysian Prison System – Zenerations Malaysia
[…] there is no official data on the mental health data of prisoners in Malaysia, there have been studies conducted proving the higher prevalence of mental illness among the prison population than i…. Figure 3 below illustrates this […]