By Dr. Chua Sook Ning
Mental illness is often brought up as a possible cause when an incomprehensible violent crime is committed. The authorities usually just say “mental illness” without further explanation or specification. Here are just some recent cases in Malaysia where the authorities have implicated mental illness:
Assault and arson (http://malaysiandigest.com/news/654630-man-suspected-of-running-amok-killing-three-and-burning-down-home-remanded.html)
Gun violence (http://www.themalaymailonline.com/malaysia/article/penang-shooting-suspect-mentally-ill-with-military-background-cops-say)
Stabbing (http://www.malaysiandigest.com/news/657766-mentally-unbalanced-ex-soldier-attacks-guard-at-gong-badak-military-camp.html)
The news coverage may give you the impression that all violent crimes are committed by people with a mental illness. But mental illness is a very broad category and includes Autistic Spectrum Disorder, ADHD, Depression, Anxiety, Bipolar Disorder, Eating Disorder, Learning Disorders, Pain Disorders and Schizophrenia spectrum disorders.
Vague descriptions lead to negative generalization and increases the stigma of mental illness. As soon as you and I hear the words “mental illness” and “violence” in the same context, it creates a cognitive and emotional association.
Mental illness = violence = fear.
This leads to an emotional response of fear towards mental illness, and a negative attitude towards mental illness. Consequently we are more likely to act negatively towards people suffering from a mental illness.
This reaction is an automatic one. Understandably we avoid feared objects. However, we must rise above our automatic visceral reaction and approach this issue logically, if not with compassion if we actually want to address the issue and prevent such occurrences from happening.
1. Is there a link between mental illness and violence?
Depressive disorders do not seem to present an increased risk once substance abuse is controlled for, whereas psychotic disorders is a risk factor for violence even after controlling for substance abuse and socioeconomic status (Brennan, Mednick & Hodgins, 2000; Van Doorn, Volavka & Johnson, 2012). On average, the relationship between psychotic disorder to violence towards others is r = .12 [r ranges from -1.00 (a perfect negative relationship) to +1.00 (a perfect positive relationship)] (Douglas, Guy & Hart, 2014).
Let’s compare that with other risk factors for violence:
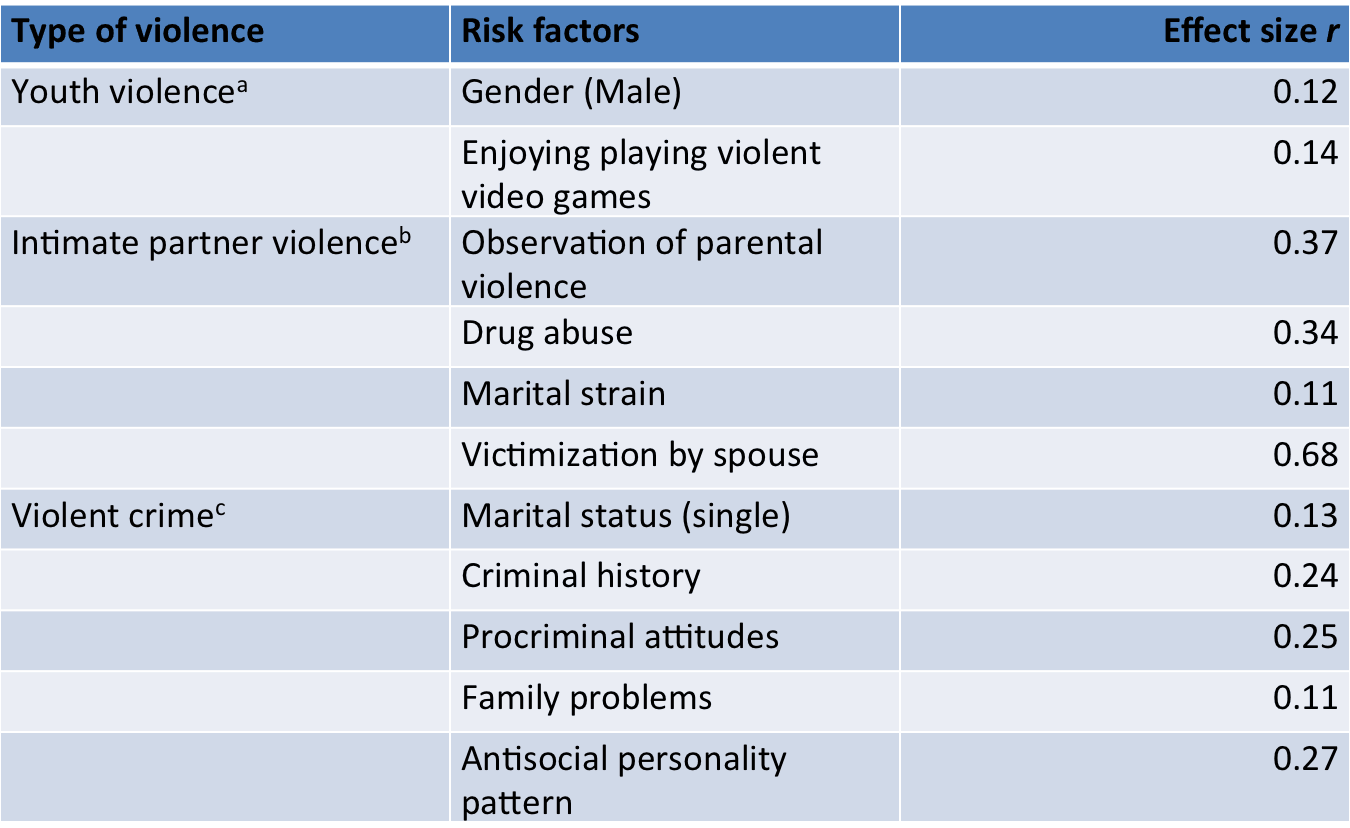
a DeLisi, Vaughn, Gentile, Anderson, & Shook, 2013 b O’Leary, Tintle, & Bromet, 2014 c Bonta, Blais, & Wilson, 2014
In reality, only 5% of all violent crimes (or 1 in 20) are committed by patients with a mental illness (usually psychotic disorders).
2. If mental illness is involved, the answer is not harsh punishment, but treatment.
Everyone should advocate for early identification, and effective evidence-based prevention and treatment programs. Patients with a serious mental illness who committed a violence offense were often not in active treatment. They tend to fall through the cracks of the system without good community based care to help them integrate into society and monitor their symptoms.
3. If mental illness is involved, the answer is not social ostracization or hostility.
A negative environment causes great stress for the patient and increases the risk of other co-occurring mental illnesses such as depression and anxiety. Stress is a high risk factor for a psychotic relapse.
If someone asked you if you wanted to increase the chances of violent crime happening, the answer is obvious -“No”.
Yet that is what we are doing if
- We continue to stigmatize and ostracize people with a serious mental illness.
- We continue not to fund the development of accessible and effective evidence-based prevention and treatment programs.
- We continue to lack mental health laws which facilitate prevention and intervention in a compassionate and autonomy supportive manner.
If mental illness is involved, we must create an environment that is helpful to the patient not one that will further harm the patient. This is the reasonable and logical response.
References
Amaresha, A. C., & Venkatasubramanian, G. (2012). Expressed emotion in schizophrenia: an overview. Indian journal of psychological medicine, 34(1), 12.
Fazel, S., & Grann, M. (2006). The population impact of severe mental illness on violent crime. American journal of psychiatry, 163(8), 1397-1403.
Perry, Y., Henry, J. D., Sethi, N., & Grisham, J. R. (2011). The pain persists: How social exclusion affects individuals with schizophrenia. British Journal of Clinical Psychology, 50(4), 339-349.
Dr. Chua Sook Ning is a Clinical Psychologist and a lecturer at the National Institute of Education at Nanyang Technological University, Singapore. She believes in raising public awareness of mental health by encouraging open and public conversations of mental health. She also is also working on early identification of mental health conditions by promoting mental health screenings and. training communities to recognize mental health conditions. Finally, she is working with a team of international researchers to develop accessible and affordable mental health interventions.




0 Comments